I never imagined that more than thirty years after entering the beauty industry inspired not by vanity, but by survival I would find myself questioning whether ethics still sit at the heart of our regulatory systems.
But here we are.
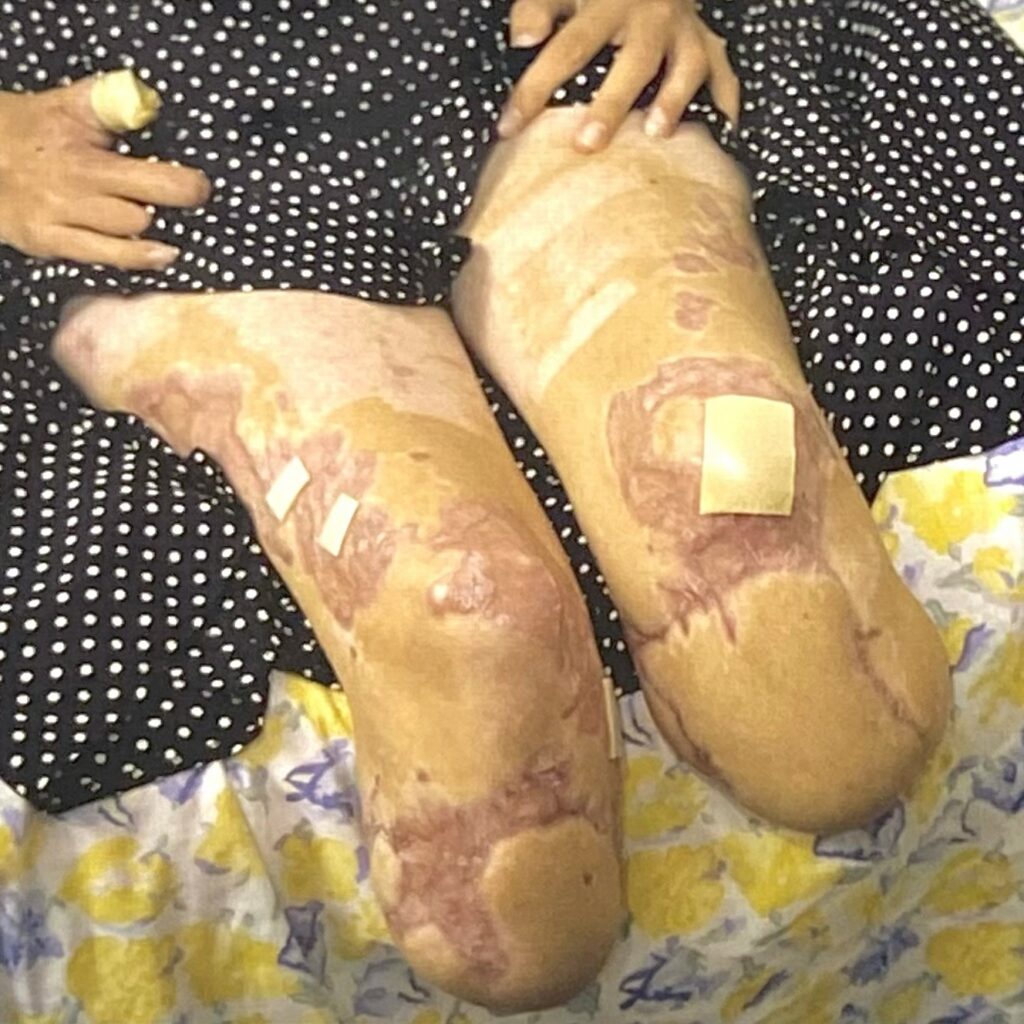
I am a sepsis survivor.
I live with amputations to both my legs.
My body carries full-thickness (Hypertrophic) scars and skin grafts that tell a story of trauma, survival, and resilience.
Those scars didn’t push me away from this industry – they pulled me towards it.
They are the reason I chose to train, qualify, and continue qualifying.
They are why I have always believed that anyone working on damaged, vulnerable skin has a moral obligation to be properly educated, regulated, and accountable.
So when I look at the current situation surrounding MCA Dry Needling, I feel not just frustration I feel genuine anger.
In the UK, a beauty therapist or medical professional wishing to work safely and legitimately on the skin is expected to complete Ofqual-regulated vocational qualifications. (VTCT, Btec, NVQ)
These qualifications:

And yet…
How is this ethical?
How is this defensible?
How is this remotely consistent?
There is another truth I need to say out loud.
One of the main reasons I made the conscious decision to move away from tattooing was the lack of regulation, the absence of meaningful qualification requirements, and the increasing overlap into aesthetics and medical-style treatments without appropriate training.
Tattooing, at its core, is an artistic profession. But in recent years, it has expanded far beyond decoration of healthy skin. Tattoo devices and needles are now being used to treat:
All without a requirement for medical or vocational beauty qualifications.
That shift deeply troubled me.
I could not ethically reconcile working in an environment where invasive procedures on vulnerable skin were becoming normalised without anatomy, pathology, wound-healing education, or regulated oversight.
I have lived in a body that did not heal normally.
I understand what happens when skin fails. I almost died – twice as a result.
And I refused to be part of a system that allows people to work on damaged bodies without truly understanding them.
So I chose a different path.
I chose regulation.
I chose education.
I chose accountability.
And yet now, the very standards I stepped away to uphold are being undermined not by patients, but by regulatory inconsistency.
When unqualified individuals are permitted to perform medical scar treatments after a one-day course, while trained professionals are restricted unless they hold Ofqual-regulated qualifications, something has gone profoundly wrong.
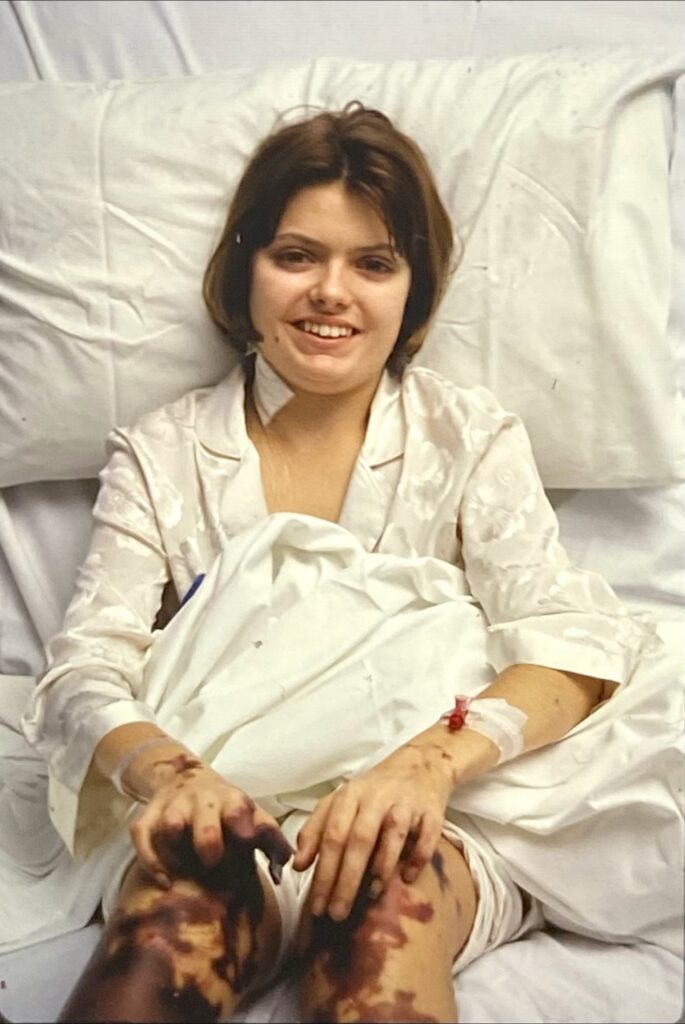
I know this is not going to be a popular post with many of my peers!
This is not about attacking tattoo artists.
This is about protecting patients.
And it is about asking why those who choose training and ethics are being held back, while those who bypass them are waved through?
I want to be clear about something else, because this matters.
I understand wholeheartedly the desire to help people.
The wish to give something back.
The genuine motivation to make a difference in someone’s life.
Many tattoo artists and trainers entering this space are not driven by harm. They are driven by empathy.
But good intentions do not replace qualification.
At some point, every practitioner and every trainer has to pause and ask themselves:
“Is this right?”
“Am I genuinely qualified to offer this treatment?”
When we are dealing with scarred, traumatised, or medically compromised skin, the ethical threshold must be higher not lower.
There is another option that too often gets overlooked.
Partner with practitioners whose expertise exceeds our own
have always believed in sticking to my area of expertise and recommending others when a client’s needs fall outside it. Not because I lack compassion but because I respect the limits of my knowledge.
Diluting expertise helps no one.
Collaboration protects clients.
True professionalism isn’t about doing everything.
It’s about knowing when not to.
Let’s be clear:
Calling MCA Dry Needling an “Inkless Tattoo Treatment” does not make it non-medical.
Yet somehow, this wording has created a loophole where non-medical, non-beauty professionals can perform scar treatments that many trained therapists are prohibited from offering without extensive qualifications.
As someone who lives in a body permanently altered by medical trauma, this terrifies me.
Scarred skin is not “normal” skin.
It does not behave predictably.
It carries higher risk.
Allowing unqualified individuals to work on it is not empowerment it is negligence.
The people seeking scar treatments are often:
The result may be:
The patient suffers not the system that allowed it.
This is the contradiction at the heart of the issue:
And competence is non-negotiable when needles and damaged skin are involved.
This is not about professional turf wars.
This is about ethics, safety, and accountability.
I also need to be clear about why I am speaking out.
Alongside my professional work, I am an ambassador for three UK charities:

These roles place me in regular contact with individuals and families who have already experienced serious illness, medical trauma, surgery, or life-altering diagnosis. Many of the people supported by these charities go on to seek scar treatment not for vanity, but for healing, confidence, and recovery.
That is why regulatory inconsistency in scar treatment standards concerns me so deeply.
I have seen first-hand how vulnerable bodies respond when care is rushed, poorly informed, or inadequately regulated. I have also seen the emotional damage that follows when people place trust in a system that fails to protect them.
My advocacy work is rooted in prevention, education, and harm reduction. Speaking out about MCA dry needling and training standards is an extension of that same responsibility.
This is not about professional hierarchy.
It is about safeguarding survivors.
If you are a patient or client reading this, please protect yourself. Ask:
A reputable practitioner will welcome these questions. Go away and research the answers.
I have spent over three decades qualifying, learning, refining, and respecting the responsibility that comes with touching another person’s skin.
My scars taught me that what we do to the body lasts.
That is why I am sharing this with:
Because silence enables harm.
And because as an amputee, a survivor, and a professional, I refuse to accept a system where the least qualified are given the greatest freedom, while those who train properly are restricted in the name of “safety”.
If safety truly matters then standards must make sense.
Right now, they don’t.
I walked away from an unregulated space because I believed safety mattered more than convenience.
The question now is whether our regulators, insurers, and licensing bodies are willing to do the same.

Legal Disclaimer (UK – Defamation-Aligned)
This article constitutes an expression of honest opinion based on my personal lived experience, professional background, and understanding of current industry practices at the time of writing. It is published in the public interest, with the sole intention of encouraging informed discussion around regulation, training standards, and patient safety.
No statement within this article is intended, nor should be construed, as an allegation of unlawful conduct, professional misconduct, or negligence by any named or unnamed individual, organisation, training provider, insurer, or regulatory body.
All references to qualifications, accreditation, insurance acceptance, and licensing practices are made in general terms and are derived from publicly available information, industry guidance, and professional observation. Regulatory frameworks and insurance criteria may vary by local authority and are subject to change.
This article does not provide medical, legal, or clinical advice and should not be relied upon as such. Individuals seeking treatment are advised to undertake their own due diligence and consult appropriately qualified and regulated professionals.
This publication is intended to promote clarity, consistency, and ethical consideration in public-facing regulation and is not directed at, nor does it seek to disparage, any particular profession or sector.







Sign up to my mailing list to ensure you receive all updates, my last minute booking availability, new products and treatments, offers and special discounts.
Happy shopping!